What is Actinic Keratosis?
Actinic keratosis (plural, keratoses) is a small, rough, precancerous growth of sun-damaged skin. Also caused by repeated use of tanning beds over a long period of time, actinic keratoses usually appear on adults older than 40 who have had sustained exposure to the sun’s ultra-violet (UV) rays. Actinic keratoses are concerning because, left untreated, some of them can develop into skin cancer. Typically once an individual actinic keratosis appears, others will follow, putting you at a higher risk.
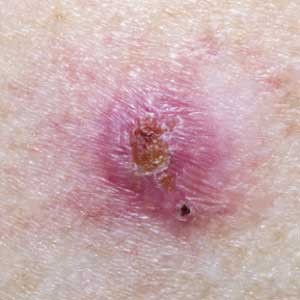
What does actinic keratosis look like?
Unlike smoother marks on the skin, such as ordinary moles, actinic keratoses are typically rough or crusty spots or patches of skin that are often slightly raised. They may resemble warts, scabs, or appear as irregularly shaped, discolored spots. They are often described as having a sandpaper texture. Actinic keratoses can appear singly or in clusters, and they vary in color from tan or brown to pink or red. Because they occur on skin exposed to the sun, they are most common on the face, forehead, lips, ears, scalp, neck, forearms, and back of the hands.
What are the risk factors for actinic keratosis?
The biggest risk factor for actinic keratoses is cumulative build-up of UV damage to the skin, i.e., too much exposure to UV radiation over a long period of time. That’s why people over 40 years of age are most affected. However, according to one recent study, the incidence of actinic keratoses continues to rise among younger sun-damaged populations as well. People with fair skin and those who live in hotter, sunnier places (as in countries closer to the equator) also carry more risk, as do males in general and balding males in particular. Increased sensitivity to UV radiation caused by other skin conditions can also make you susceptible to actinic keratosis (1).
Can actinic keratosis turn into skin cancer?
Although only about 1% of actinic keratoses become skin cancer, there is a strong association between actinic keratosis and squamous cell carcinoma (SCC) (1), one of the three main types of skin cancer.
To determine if actinic keratosis is cancerous, some dermatologists use a 3-tiered classification system based on the presence of abnormal, or atypical, cells in the lowest layer of the epidermis (this is called basal atypia). This abnormality in the cells can move upward through the entire thickness of the lesion. However, not all actinic keratoses behave this way. In fact, many lesions will stay in the first benign stage or even regress, while only a few will turn into SCC (2). The critical determination is whether the abnormal cells are present only in the lower levels of the lesion of if the entire thickness is affected, and only your doctor will be able to distinguish the difference.
The good news is that the estimated annual risk of progression from actinic keratosis to SCC for an individual lesion is believed to be small; still, the cumulative risk for a patient with multiple lesions over time is substantial (1).
What should I do If I suspect I have actinic keratosis?
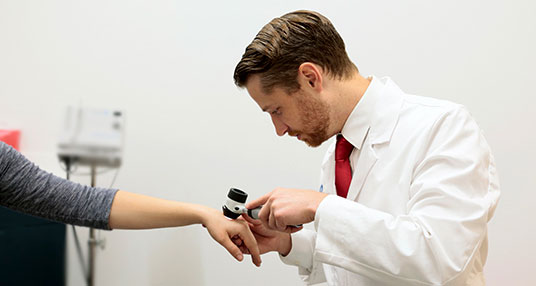
Once detected, early identification of the actinic keratosis by a dermatologist is critical to reducing risk. This is especially important for actinic keratoses that appear on the head or neck, the site of more aggressive skin cancers. Confirming that the crusty bump that’s appeared is indeed actinic keratosis will allow your doctor to monitor its development, check for any new lesions, and prescribe the most appropriate treatment.
Final Word on Actinic Keratosis
As the old saying goes, “An ounce of prevention is worth a pound of cure.” To reduce further development of actinic keratosis, be proactive in developing common-sense practices for your outdoor activities. Minimize your sun exposure when the UV rays are most intense, and refrain from tanning altogether, whether in the open air or in a tanning booth. Learn about other measures to protect against sun damage to your skin. It’s worth it in—and for—the long run.
Suggested Resources
American Academy of Dermatology
Articles Cited
- Hashim PW, Chen T, Regel D, et al. Actinic keratosis: current therapies and insights into new treatments. J Drugs Dermatol 2019;18(5 Suppl 1):s161-166 Accessed April 21, 2021 at https://jddonline.com/articles/dermatology/S1545961619S0161X
- Fernandez Figueras MT. From actinic keratosis to squamous cell carcinoma: pathophysiology revisited. J Eur Acad Dermatol Venereol (JEADV) 2017;31(Suppl 2):5-7. doi:10.1111/jdv.14151
- Mane S, Singer J, Corin A, et al. Successful treatment of actinic keratosis with kanuka honey. Case Rep Dermatol Med 2018; 4628971. Published online 2018 May 31. doi: 10.1155/2018/4628971.
Saguaro Dermatology Reviews

Itaro Elaisa
“I totally recommend this place to anyone who’s looking for a dermatologist who’s professional, informative, respectful and very helpful. They are quick to solve your problems and get you home.”

Wendy L.
I had an awesome experience with Dr Hamann and staff. I was very comfortable and i was able to have all my questions answered without feeling rushed. The staff was courteous and welcoming.

Robert P.
Staff was friendly, & on time. office is super clean!! Doctor was awesome, felt like a family member taking care of me.

Kristin U
“Dr Dathan and the team were very helpful, kind and knowledgeable. Plus, there was no wait time so I was able to get back to work faster than expected. I would highly recommend.”

Amanda C.
Great doctor and friendly, professional staff. The doctor spends time listening and answering questions, something rare to find anymore. The office is beautiful and very clean. I love all the artwork with saguaros.

Sally S.
“Very friendly and professional. I had a great experience, Dr. Hamann was very good at answering my questions and concerns. I will certainly come back for another visit.”

Kylin L.
“The office was recently renovated–it is a beautiful, clean, and calm environment. I would highly recommend this practice for anyone who is looking for a general dermatologist.”

L
Dr. Hamann is very knowledgeable, nice, and professional. You can tell that he truly cares about his patients by the way he operates. He took the time to listen to all of my concerns then address them with good, well-informed answers.
About Saguaro Dermatology
Our comprehensive dermatology clinic is dedicated to providing you with the highest quality of care, innovative practices, helpful resources and state-of-the-art technology to prevent and treat a multitude of skin disorders. Led by Carsten R. Hamann, MD, PhD, Dathan Hamann, MD, FAAD, Michael McBride, DO, Millard Thaler, MD, Mohs Surgeon and Jenna Wald, MD, Mohs Surgeon, our passionate team looks forward to serving you with respect and compassion.
 Ahwatukee
Ahwatukee